admin
Latest posts by admin (see all)
- Wart Cream: Which One to Choose? - October 14, 2019
- Wart Freeze: How Does the Cryodestruction Take Place? - October 11, 2019
- How to Use Salicylic Acid for Warts Removal? - October 8, 2019
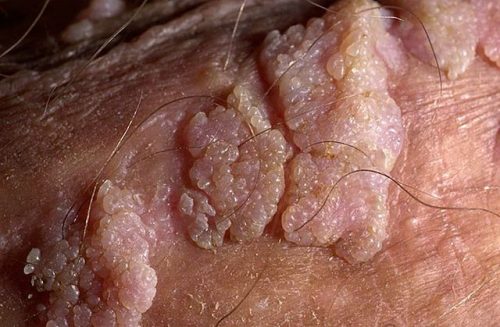
Genital warts are warts that can grow on the skin around the anus (anal warts), as well as on the mucous membranes of the genital organs or mouth. They appear as a result of infection with the human papillomavirus (HPV). This infection is quite common in the world and most often external manifestations can only be warts on the genitals. There are cases when this seemingly innocuous disease can lead to oncological complications.
Contents
- Causes of Genital Warts
- The Main Distinctive Symptoms of Genital Warts
- Classification by Localization
- How to Diagnose Genital Warts?
- How Can You Get Infected?
- Factors that Create Favorable Conditions for Genital Warts
- Possible Oncological Complications of Having Genital Warts
- Is It Possible to Treat Genital Warts Effectively?
- Precautions and Prevention Methods
Causes of Genital Warts
The causative agent of genital warts is a human papilloma virus of a certain type. Modern medicine identifies about 100 different types of HPV but the viruses of a certain type are responsible for the appearance of warts in intimate places. Infection in most cases occurs sexually, much less often – through household items.
HPV types that cause Genital warts: 6, 11, 30, 40-45, 51, 52, 54.
Therefore, if a person has a genital wart, then during the treatment doctors do not recommend to live a sexual life, because even with the use of contraceptives, infection can be transmitted. In the process of sexual intercourse, infection from an infected person gets on the mucous membranes of a healthy person, and if there are wounds or microcracks, the virus gets into the skin cells and subsequently papillomas can appear on these places.
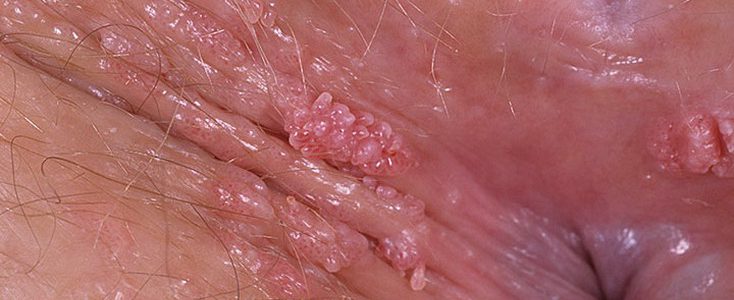
The incubation period of the virus lasts from several weeks to several years. A strong immune system will suppress the infection, although the virus does not disappear from the body. No external manifestations will be observed. If immunity is weakened, warts will appear on the genitals.
The Main Distinctive Symptoms of Genital Warts
During the period of carrier infection, the presence of the virus can only be confirmed by laboratory tests. There are no visible symptoms at this stage. The subclinical form of genital warts can be detected by carrying out all necessary examinations and analyzes. When clinical signs manifest themselves, diagnosis is no longer a problem.
There are three forms of the disease:
- carrier of the virus;
- subclinical manifestations;
- clinical manifestations.
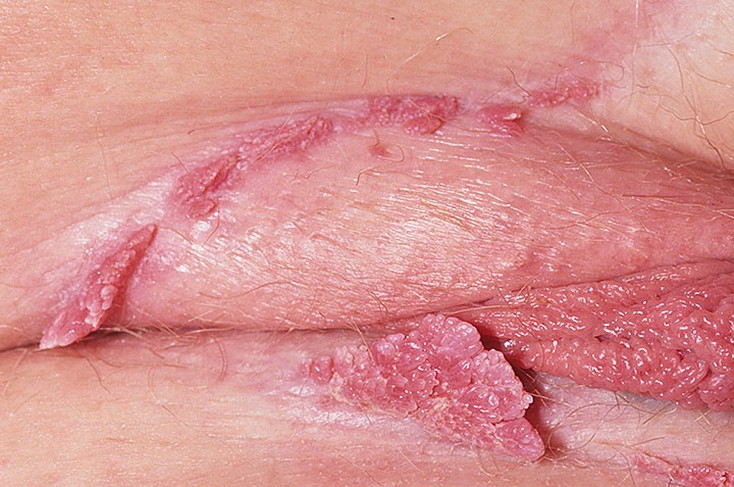
At the first stage of the disease, a small rash of a reddish shade appears on the skin in the genital area. The rash lasts about two weeks. After that they turn into sprouting by the type of cauliflower flat or irregularly shaped. They can be multiple or single. The length is from 1.8 mm to 10 cm in contrast the size of common warts varies from 5 mm to 1-1.5 cm .
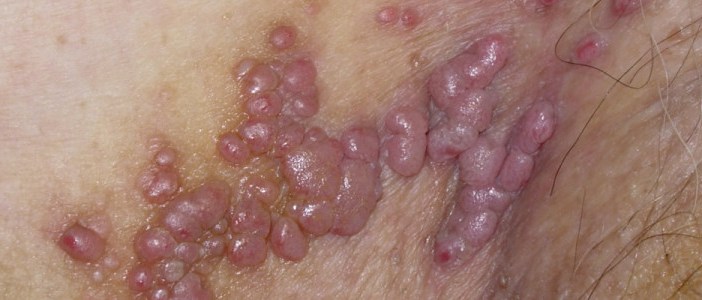
In women, warts are usually located in the vagina, anus, labia, and vulva. Sometimes genital warts are formed on the cervix. In men, genital warts occur on the scrotum, in the anus, and on the glans penis.
To children they can be transferred from a sick mother in the process of childbirth (transplacental path). In this case, these warts can form in the child even in the throat or any other parts of the body.
Such warts are accompanied by severe itching, redness, and inflammation of the skin. In some cases, bloody or white discharge from the genitals can be observed. There are painful sensations during sexual contact, urination is impaired.
Classification by Localization
Warts are classified according to the place of formation. They can occur not only on the genitals, but also on a number of located areas: in the groin, on the pubis.
The female organism suffers from warts in such zones:
- in the labia (on large and small);
- at the entrance or inside the vagina;
- in the cervical region;
- around the anus;
- in the urethra.
Men often have warts on the penis, but there are also places of common localization:
- the outer side of the anal passage;
- on the internal parts of the urethra;
- under the foreskin;
- in the region of the scrotum.
How to Diagnose Genital Warts?
In order to identify the human papillomavirus and put a correct diagnosis, a number of activities are carried out:
- examination of the patient;
- PCR;
- the cytological method;
- molecular-biological test;
- histological method.
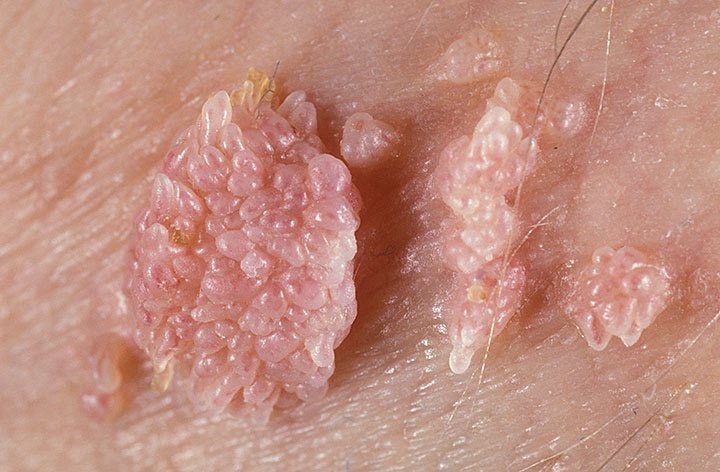
Genital warts should be differentiated with manifestations of secondary syphilis, since they have similar symptoms. A simple examination of the genitals can be carried out with the help of a colposcope and differential dyeing of the skin in places where warts accumulate. Cytological diagnostic method refers to more in-depth and more complex methods. It allows you to identify a precancerous condition and assess the degree of tissue damage. Laboratory methods can reveal the type of the papilloma virus.
To detect the disease even before the manifestation of the first clinical signs can be using a molecular biological method that allows for accurate identification of the virus. Testing is carried out with the help of special biomarkers, indicating changes in cells or oncoproteins. Also, at the stage of carriage of the human papillomavirus virus, PCR (polymerase chain reaction method) can be performed. Thus, the type of the virus and the degree of oncogenicity are revealed.
How Can You Get Infected?
The most common way of infection is sexual contact with an infected person. HPV and the diseases caused by it – phenomena widespread all over the world and among all layers of the population.
Important: Only 1-2% of the carriers of the virus have skin lesions.
Rare can be called cases of infection with genital warts by the household way or in medical institutions. To establish that this way the virus got into the body is very problematic. Genital warts in some cases are observed even in infants. During childbirth, the virus from an infected mother can reach the newborn. As a result, the child may develop neoplasms on the genitals.
Factors that Create Favorable Conditions for Genital Warts
Unfortunately, it happens that appearance of warts on genitals can signal the presence in the body of not only HPV but also other diseases transmitted sexually.
To such diseases, it is possible to refer:
- mycoplasmosis;
- urogenital chlamydia;
- bacterial vaginosis;
- cytomegalovirus infection;
- herpetic infection.
As a result, the treatment of both the papilloma virus and the concomitant disease is complicated. The likelihood of recurrence increases, cure will also take a longer time. It is impossible to cure HPV completely, you can only get rid of the symptoms. Under certain conditions, there is always a chance of a relapse.
These conditions can be:
- weakening of immunity, for example, as a result of illnesses or a lack of vitamins;
- promiscuous sexual intercourse and disregard for the use of contraception (although it will not give a full guarantee of protection, but will significantly reduce the risk of infection);
- other sexually transmitted infections;
- hormonal failures in the body;
- pregnancy;
- the use of intrauterine contraceptives;
- medical intervention (abortion, etc.).
Possible Oncological Complications of Having Genital Warts
When the virus enters the body with weakened immunity, in most cases this leads to benign formations on the genitals. Not every type of HPV has high oncogeneity. In general, the trouble is only in the appearance of warts on the penis in men or in intimate places in women.
There are types of the virus (16 and 18) with a high degree of oncogeneity. The ability to cause cancer in the papillomavirus was discovered relatively recently, it was previously thought that HPV does not lead to cancer complications.
Important: Most often, cervical cancer, the cause of which can serve as genital warts, is found in women with promiscuous sexual intercourse.
In the risk group, there are those who early began to lead a sexual life. In addition, women who have genital warts abuse cigarettes and alcohol. The development of the virus occurs faster and the immune system becomes weaker. Often from the moment the first papillomas appear before they are detected, a fairly long period of time may pass. This is especially true of women, because genital warts, for example, on the cervix cannot behave in any way. Only a doctor or a Pap smear test can detect them. That’s why one cannot neglect planned examinations at a gynecologist, especially those who often change their sexual partners and ignore contraceptives.
Don’t panic much and assume that you will certainly get cancer if you have found genital warts. A lot of time must pass for the regular genital wart to become malignant. The doctor in a timely manner will detect an oncological disease and offer treatment. Cervical cancer at an early stage is almost always curable.
Is It Possible to Treat Genital Warts Effectively?
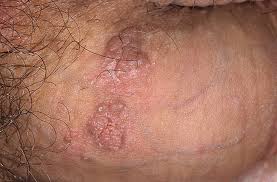 Up to the present moment, there is no medicine capable of relieving HPV in the body. It is only possible to eliminate the symptoms of the disease – anogenital warts. You can physically remove them in several ways. In addition, doctors recommend drugs that slow the spread and development of the virus in the body.
Up to the present moment, there is no medicine capable of relieving HPV in the body. It is only possible to eliminate the symptoms of the disease – anogenital warts. You can physically remove them in several ways. In addition, doctors recommend drugs that slow the spread and development of the virus in the body.
In general, warts in intimate places can disappear themselves, without any treatment. And although the virus of the papilloma will remain forever in the body, it can never disturb its carrier again.
Important: In 50% of infected, who have been found sex warts, relapse no longer arose. However, according to statistics, in one of the four patients, they appear again within the first three months after removal.
Treatment for each patient who has found venereal warts, the doctor selects individually. This takes into account the general condition of the patient, the presence or absence of other sexually transmitted infections, and other factors. Now basically doctors use complex treatment, when not only physically remove papillomas, but also immunostimulating and antiviral drugs are prescribed. All information about genital wart treatment you’ll find here.
Main methods to remove warts:
- Cryotherapy, or exposure to liquid nitrogen. This method removes warts on the penis or near the vagina. It is used to get rid of small growths. The patient should avoid sexual contact until healing, until the tumors come off.
- Surgical excision. Under local anesthesia, anogenital warts are simply cut with a scalpel. This method is not suitable for large formations, because after excision, scars may remain.
- Electrosurgical method. It is used in cases when genital warts are large. Specimens heated by special heated device under anesthesia (local or general).
- Laser surgery. This method uses a medical laser to remove large warts, or located in hard-to-reach places, such as the urethra or inside the anus.
- Diathermocoagulation. Genital warts are cauterized by high-frequency current using a special device.
- Chemical method. Removal is carried out with nitric or trichloroacetic acid, also use pherezol and solcoderm.
Along with the removal of genital warts, the doctor may prescribe antiviral and immunomodulating medications. Cytotoxic drugs are podophyllotoxin; podophyllin; 5-fluorouracil. Interferons, such as cycloferon or laferon, are used as medications used to strengthen the immune system.
There are a number of hygienic recommendations for a person who has noticed genital warts. You should avoid using soap and other products with odors and flavors. After washing, the genitals should be well dried with a towel, since a moist environment is favorable for viruses, bacteria, and fungi. Do not wear synthetic clothes, and you should also avoid rubbing your skin. In addition, the underwear should be changed every 6 to 8 hours, and it should be washed separately from the rest of the clothes.
Precautions and Prevention Methods
- Do not use any medication yourself without consulting a specialist. It should be remembered that in the absence of treatment genital warts or condylomata are able to pass into malignant formations and give relapses.
- It is necessary to avoid accidental sexual intercourse and always use protective contraception.
- It is necessary to enhance the immune system with the help of special drugs, exercise, and proper nutrition.
- It is necessary to treat viral and infectious diseases on time. It is necessary periodically to undergo examinations in medical institutions and consult a doctor noticing the first signs of warts.